Blood donation process must stop discriminating by sexuality
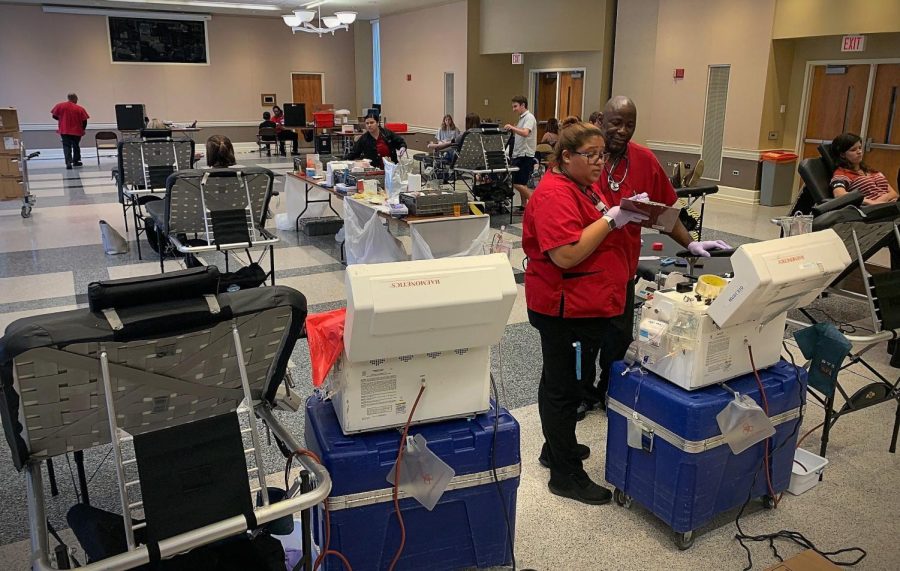
A university blood drive run by the American Red Cross.
Why does a lifesaving process discriminate based on sexuality?
That question casts a dark shadow over the process of blood donation in the U.S., impacting otherwise-positive efforts such as the Cherry Hill High School East annual blood drive.
In the U.S., the government’s Food and Drug Administration regulates blood donation. One of their regulations prohibits men who have had sex with other men from donating blood for three months after each instance of sexual activity. Until 2020, the “deferral time” was an even longer period of one full year after sex. For LGBTQ+ men who are consistently sexually active, this discriminatory restriction may prevent them from ever donating blood.
Such restrictions harm not only discriminated-against LGBTQ+ people, but also all people who may ever need medical care involving blood transfusions. With a blood availability crisis ongoing, blood donors are needed more than ever. Losing out on countless potential donors by discriminating against them only worsens the crisis.
So, why are such harmful regulations in place? It all goes back to the HIV/AIDS crisis in the 1980s, which spurred concerns that gay men would transmit the virus through blood donation. At the time, public information about HIV/AIDS was limited and misconceptions abounded. Today, significant advancements in medical understanding of the virus have been made. Plus, blood screening technology has improved to detect HIV/AIDS before donated blood is used.
According to the American Medical Association (AMA), a professional group for doctors and medical students, the restrictions were created “in an era when HIV was poorly understood [and] persisted for decades even as blood-screening technology improved dramatically.”
The AMA and the American Red Cross, a nonprofit organization responsible for around 40% of blood collected in the U.S., both support proposals to do away with any kind of categorical ban that prevents men who have sex with men from donating blood. Instead, the AMA proposes that the FDA should develop a new process that requires more thorough, holistic evaluations of each potential blood donor’s individual risk factors, instead of using categorical determinations. These regulatory updates would better protect all people based on modern medical best practices.
Until then, blood drive organizers must remain sensitive to LGBTQ+ perspectives on donating blood. Men who have sex with men may not feel comfortable sharing their sexuality when asked why they can or will not donate blood. As such, organizers should take “no” for an answer and respect all individuals’ personal choices to donate or not donate blood. Then, they and all other citizens should advocate for the FDA to change its regulations in accordance with AMA guidance as soon as possible.

Elle Rood is a sophomore and Eastside Global Commentary Editor. Outside the (virtual) newsroom he can be found staffing national political campaigns, collecting...