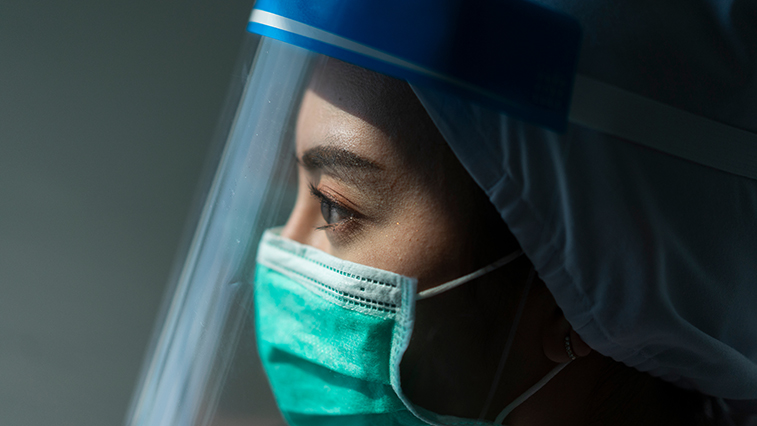
Healthcare perspectives
October 28, 2021
Many healthcare workers are struggling with the new way of life at work caused by the pandemic.
Alexa Albert
Alexa Albert has been a registered nurse in cardiology for the past twenty years. Interestingly enough, not only has Alexa’s work changed due to COVID, but COVID has become her work. Through specializing in the COVID unit, Alexa became a traveling nurse in February to support the high demand for frontline workers. She explained this process, but simply put, she works in each designated location until her contract is up. Alexa works twelve to sixteen hours every day.
Usually, each contract lasts a few weeks at a time. Safety is a top priority for those working in the COVID unit so, Alexa said she wears a gown depending upon the time duration each nurse stays with the patient. Alexa wears a level four gown being that she spends the longest duration of time with patients. Gowns are numbered one through four, with four being the most protective and restrictive gown. They also wear headgear similar in appearance to a biker helmet. Protecting her face is a shield and an N-95 face covering. Some of these clothing restrictions include the tight sealing that exists with such protective uniforms. The uniform lets in such little outside air, so, nurses find their eyes getting red and dry. It is very difficult for these nurses to get water as they have to remove the entire suit to do so. Alexa shared that something her unit has been doing is making their nurses print a picture of themselves and attach it to the outside of their suit. This way, the patient can see the faces of the nurses all suited up for protection. “The COVID unit is a no visitor allowed area. As morbid as this is, the only area with visitors allowed is for dying patients. And even then they need to be in a suit as a visitor and are only allowed in for a short duration. Overwise, it’s staff only in these units,” said Alexa.
For her, she finds working as a Covid nurse during these unprecedented times has isolated her from her family. “A lot of people don’t realize everyone in my department is actually fully vaccinated and we are fully covered from head to toe, but my friends, where you know, nervous to be around me knowing what I do. It’s sad and lonely to wake up at 4 in the morning, be in a gown all day, can’t eat at the same table at lunch with other nurses, get home until 8:30 at night, and not be able to see friends and family. But I love being able to help.”
She shared with me that she’s grateful to see the effects of the vaccine. “People think the vaccine is political. It’s just been proven to me that working with patients in critical care every day, those that are fully vaccinated heal faster and are much safer than those who didn’t get the vaccine. Being that I work to rescue patients like this, I just see those that are vaccinated having greater survival rates in the hospital. Either way though, whether the patient is vaccinated or not, I honor them and care for them just as good. That is our job.” Alexa said a change from the start of COVID to now is that there has been an increase of younger patients in the Covid unit. She suggests staying physically active and working. “It helps the lungs to open up. Also, people should look to educate on getting vaccinated. But if anyone is experiencing signs of COVID, they should isolate themselves at home and seek medical attention.
MARISA RILEY PIZZI
Marisa works at a private practice in primary care pediatrics as a physician assistant. She has been a PA for the last six years but worked in medicinal research prior, meaning she has spent the last ten years in the healthcare industry.
“Covid has affected work in every single possible way, including just the basics of how I get ready for the day,” said Marisa. Prior to the pandemic, she said it wasn’t uncommon for physician assistants to dress as they pleased. “I used to actually wear real clothes, and try to look nice at work. And now I wear scrubs every day,” said Marisa. In addition to the unified scrubs, all employees in her office must wear an N-95 mask and eye goggles.
Despite the changes in attire, Marisa notes that the biggest change is simply how often COVID is the topic of conversation. “Pretty much every one of my visits talk about COVID in some way. So whether it’s someone that’s there for their annual physical because they’re 13 years old, which happens regardless of COVID, we often talk about if they had COVID in the past two years. Or if a child has a fever, even though I think it’s an ear infection, is it an ear infection because they had a viral illness that was COVID?” Whether it is a small part of the visit or not, Marisa says she cannot remember a time since the start of the virus where it was not mentioned at least once in a session. Her office is also now requiring patients to wait in their car instead of in a waiting room.
Additionally, different times of the day are meant for different types of visits. Those that are going for well-visits enter in the mornings. Those that are sick must schedule an afternoon appointment. “Before we used to just mix it up where everyone comes when they want. Now, we have times of the day dedicated to separating those that are sick and those that are healthy, to avoid any cases of incidental transmission,” said Marisa. While there are no mandates for COVID restrictions implemented in her office, Marisa said everyone she works with decided to get the vaccine. Another struggle for frontline workers has been limiting their emotional responses to people that complain. “I feel like a lot of parents are very frustrated with the global pandemic, as am I. Sometimes policies are frustrating to them. And I feel like as healthcare workers, we’re often the people that parents will criticize.” Somewhat jokingly, Marisa pokes fun at these types of situations that she goes through on a daily basis: “I’ll have parents say things to me, ‘So you’re telling me that I had to take off the next two days to stay home with my kid because there’s like chance that it might be COVID.’ Like, yes, that’s exactly what I’m saying.” She finds these situations awkward but says it is her job to go along with the guidelines set in place by the CDC.
While no official rules were put in place for workers to separate themselves during lunchtime, that has seemed to be the pattern at Marisa’s workplace. “It is our job to care for those with COVID, so generally people don’t congregate in the lunchrooms or hang out without masks outside of work, simply because it’s what we believe in,” said Marisa. “I already am someone who spends my time giving vaccines to kids because that’s part of general primary care pediatrics, so I already knew vaccines work. But, it’s nice to have reiteration on that,” said Marisa. Building on this, the second biggest takeaway from all of this is the changing nature of medicine. Marisa says she needs to be prepared with answered questions anytime a parent raises a concern. “Parents read something on a bulletin board on Facebook and it’s my job to give them the specific data on why that is correct or incorrect, not just say, well, there wasn’t a you know that’s not true. I should be able to prove it with data.” Her final statement was this- “whether you agree or not with the words of a healthcare worker, what they said always comes from a place of trying to do what we think is the safest thing for the patient.”